
Innovations Feed
White Papers
Biomarkers white pages
Tele-Urgent Care
Linking urgent care patients to ed usacs Clinicians through a health system-based telemedicine program
Behavioral Health Innovation
ED-based therapy with licensed social workers, a less sedating medication strategy, and timely tele-psychiatry improves care and reduces avoidable admissions
Tele-Triage in Emergency Departments
Improving the timeliness and safety in EDs through telemedicine
After Discharge Assessment of Patient Transitioning (ADAPT)
Early digital engagement after discharge solves two blind spots in ED care: ensuring safe transitions & delivering real-time Clinician feedback on patient experience
Addressing the Opioid Epidemic
Reducing opioid prescribing by ED Clinicians through education, a digital dashboard, and 1:1 feedback
Tele-Intensive Care Units (ICU)
Improving the efficiency of icus through telemedicine
Promoting Value by Improving Decisions Through Evidence (Provide)
PROVIDE - Hardwiring evidence-based decision making in emergency department (ED) care
Emergency Medical Services Telemedicine
Identifying and treating 911 patients through telemedicine
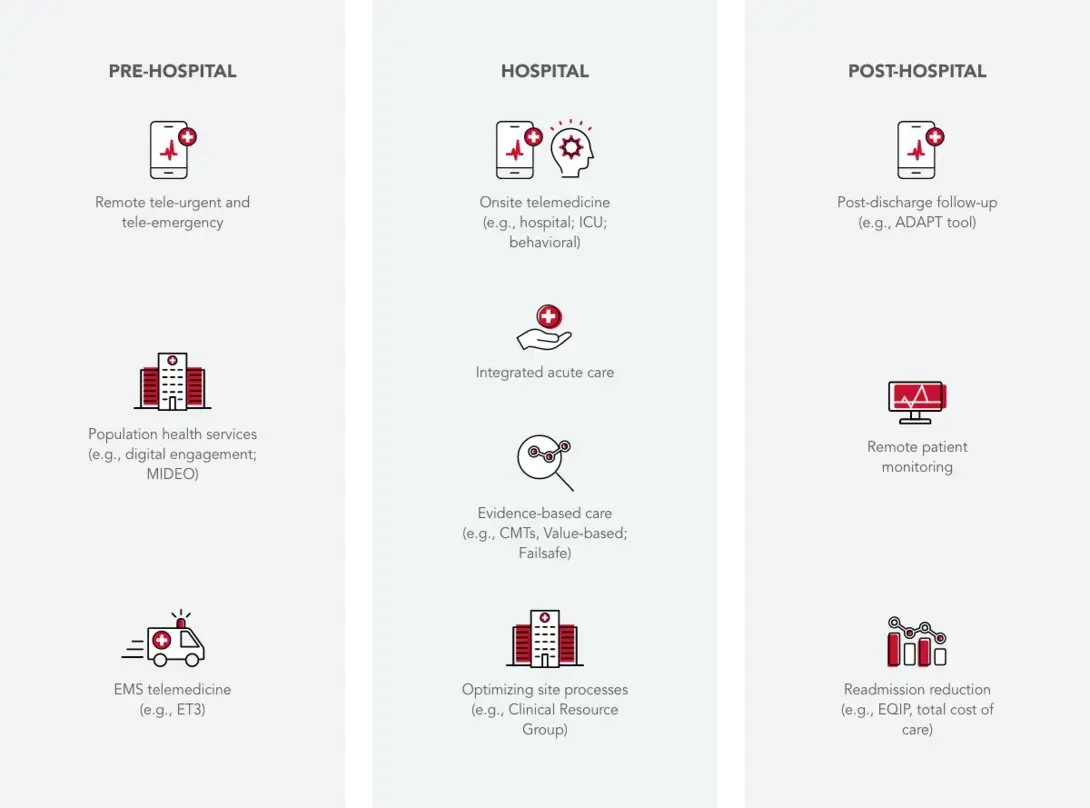
Pre-Hospital
Remote tele-urgent care and tele-emergency services allow USACS Clinicians to bring their clinical skills to the patient’s home, treat minor conditions, and help make decisions about whether to seek emergency care. Population health services involve innovative digital programs in partnership with insurance plans connecting USACS Clinicians directly with patients.
MIDEO (My Informed Decision on VidEO) is an advance care planning platform that allows individuals to communicate healthcare wishes on video and ensure proper documentation in the electronic health record aligning advanced directives with clinical care.
Emergency medicine services (EMS) telemedicine programs allow pre-hospital providers to connect in real-time with USACS Clinicians to avoid emergency department visits, when possible, and is supported by the federal government’s ET3 (Emergency Triage, Treat and Transport) model.

Hospital
Onsite telemedicine programs reduce in-person staffing costs as remote hospitalists and ICU Clinicians can deliver services more efficiently across multiple sites. USACS partners with Array Behavioral Care, a behavioral health telemedicine company to offer an innovative ED behavioral health model with remote psychiatrists, condition-specific protocols (e.g., less sedation) and ED-based counseling by therapists.
The Behavioral Emergency Stabilization and Treatment (BEST) program shortens ED length of stay and increases safe behavioral health discharges. The USACS Integrated Acute Care programs align ED, hospitalist, and ICU Clinicians in a collaborative care model that reduces interpersonal friction and improves quality through shared values and standardized pathways (e.g., a one-team approach). USACS promotes evidence-based care through its robust CMTs (Clinical Management Tools), which are evidence-based protocols designed to standardize decision-making around diagnosis and treatment.
CMTs are used in programs aimed to improve value. Specifically, USACS PROVIDE (PROmoting Value by Improving Decision through Evidence) programs combine CMTs with clinical dashboards aimed at specific goals (e.g., reducing avoidable admissions or imaging). USACS helped lead the development of the first-ever government shared-savings model in the state of Maryland aimed at reducing 14-day total cost of care for episodes of care in the Medicare population.
The USACS Failsafe program reduces risk by offering 24/7/365 second opinions for high-risk clinical situations (e.g., discharging patients with tachycardia). In the 17,000+ second opinions in Failsafe, there have been zero malpractice claims. The USACS Clinical Resource Group (CRG) delivers intensive on-site process improvement. CRG focuses on improving patient experience, promoting nursing leadership, and optimizing ED flow.

Post-Hospital
Post-discharge follow-up programs are aimed at identifying and remediating clinical issues that arise in the high-risk post-acute period after leaving the ED or hospital.
The After Discharge Assessment of Patient Transition (ADAPT) is a USACS-owned digital tool that emails and texts patients to assess the clinical experience, identifies post-discharge concerns (e.g., trouble with follow-up, filling medications, or unexpected clinical events), and deploys site-level communication to address issues.
Remote patient monitoring programs provide longitudinal care for discharged patients from the hospital, identifying and intervening on dynamic clinical issues for chronic illness (e.g., weight management in heart failure or blood pressure control).
Readmission reduction programs involve a dedicated nurse staff that communicates with high-risk patients after hospital discharge. These programs are often paired with shared savings models or hospital-based quality incentive programs.
For example, the Maryland Episode Quality Improvement Program (EQIP) program aims to reduce total cost of care in hospital discharges with acute myocardial infarction and hip fracture.

Meet the Clinical Innovation Team
World class leaders in the health care industry choose USACS. We’re proud to have a dedicated team of innovation experts that work to improve our patient-centered care.
Clinical Topics:
Leadership Topics:
Education Topics:
Research & Publications
At USACS, we invest in the future of health care with cutting-edge research that fuels insights, innovation and knowledge. By sharing our insights, we can improve the well-being for people around the world.

Fellowship Program
USACS hosts one-year fellowship programs in Clinical Innovation in emergency medicine and hospital medicine. The fellowship is intended to build the next generation of leadership within USACS. For questions about the Clinical Innovation fellowship, please contact Dr. Jesse Pines - [email protected].
