Case Study: Restoring Community Care
Case Study

The Challenge
Nonprofit health system partners with USACS to rapidly restore high-quality emergency care at four Arizona community hospitals.
In November 2024, a nonprofit health system selected USACS as its partner to help turn around care at four Arizona Emergency Departments (EDs) it had recently acquired that were in disrepair and struggling to remain open after years of poor management. Together, the health system and USACS invested in the clinical team and refocused operations on efficient, quality patient care. Five months after the February 2025 transition, each ED had seen steady improvement in every key metric. The average gains across all four sites included:
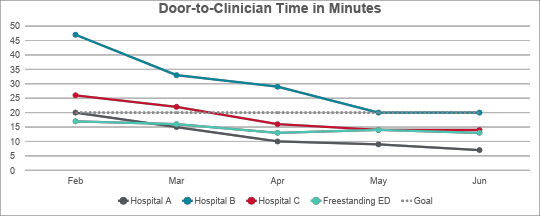
- 50% reduction in door-to-Clinician times
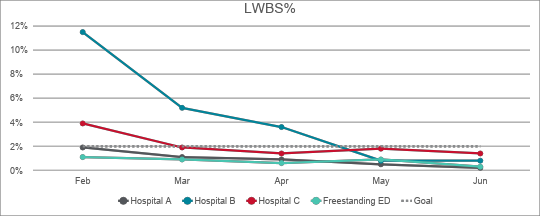
- 85% reduction in the percentage of patients who left without being seen
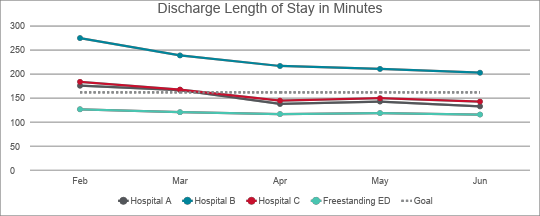
- 22% reduction in discharge length of stay
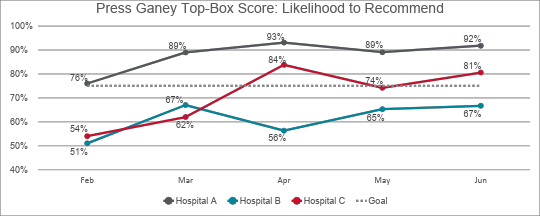
- 33% increase in patients’ likelihood to recommend the EDs
When a large private equity-backed for-profit healthcare company declared bankruptcy in May 2024, the fate of its hospitals in Phoenix’s East Valley region was uncertain. In September, a nonprofit healthcare system that then owned six hospitals in the Phoenix and Scottsdale areas announced that it would assume operations of three of the struggling East Valley hospitals and one freestanding ED.
The health system took over the severely under-resourced facilities in October and temporarily closed portions of the hospitals that required repairs, additional staff, or new equipment to safely operate. The EDs remained open; to ensure continued emergency care for East Valley communities, the health system temporarily added the Emergency Medicine Physicians and Advanced Practice Providers (APPs) to its payroll. However, the health system was not set up to employ Clinicians long-term. It needed a motivated partner with proven expertise in Clinician management functions who would provide strong leadership and be a lock-step collaborator in rapidly improving performance and restoring community confidence.
Prospective partners were allowed to conduct town hall meetings to get to know the incumbent Clinicians and understand what they would need to be successful. In November, the health system selected USACS as its Emergency Medicine partner, with a plan to transition Emergency Medicine services at all four sites on February 1, 2025.
The Solution
The health system did not wait for USACS’ arrival before making positive changes. Faced with chronic inpatient boarding in the ED, system leaders set the expectation from day one that the ED, case management, and Hospital Medicine teams should begin working together to move the patient toward the next phase of care as soon as disposition is determined. The health system recruited strong nurse leaders from its legacy sites to lead the East Valley nursing teams and fill nursing vacancies with candidates with at least three years of ED experience.
“The Clinicians needed to know that they had staff that understood the difference between sick and not sick,” says the Clinical Nursing Director at one of the East Valley hospitals. “They needed to know that when a nurse said, ‘I need you to come in here,’ they meant it.”
USACS’ initial priority was to recruit and retain both Medical Directors and as many Clinicians as possible. Thanks to the practice’s world-class benefits and Physician-ownership model, 95% of invited Physicians and 100% of APPs chose to stay. USACS’ human resources, scheduling, and credentialing departments worked hard to onboard about 40 incumbent Physicians and APPs in less than 90 days.
Before the contract was signed, knowing there would be clinical vacancies, USACS Regional Vice President Kendall Rockler, MD, FACEP, notified the practice’s Strategic Traveling Ambassador Team (STAT) of a possible deployment. USACS STAT Traveling Physicians provide auxiliary clinical support during contract transitions. Every Physician on the team has significant experience supporting new start-ups, understands USACS’ high standards and clinical management tools, and is a committed owner in the practice. Known for efficiency and excellent patient experience, the STAT Traveling Physicians’ strong performance typically helps encourage and motivate permanent Clinicians at new sites. In Arizona, the STAT Traveling Physicians worked beside the incumbent Physicians and APPs to provide high-quality emergency care while USACS continued recruiting full-time Clinicians to round out the team.
With a strong care team in place, USACS and the health system immediately invested in ensuring the Medical Directors had the operational support to drive rapid change. The health system trusted USACS’ expertise and was quick to infuse its own resources wherever necessary to help, including implementation of a Power BI dashboard that enabled the ED Medical Directors to better monitor performance at their sites.
The health system brought in leaders from its flagship hospital in Phoenix to evaluate throughput at the four new sites. Meanwhile, USACS deployed its Clinical Resource Group (CRG), an in-house consulting team of nurses and engineers who visit individual EDs to identify opportunities to sustainably improve patient flow. Together, USACS and health system leadership worked with the Medical Directors and nursing leaders to change the culture in the EDs and set the expectation that patients should be seen by a Clinician as quickly as possible. The initial goal of focusing operationally on a more efficient front-end process was to reduce the percentage of patients who left the ED without being seen (LWBS), which had climbed above 11% at one site. In a matter of weeks, LWBS dropped dramatically. As so often happens, Rockler says, other metrics followed suit.
The ED Medical Directors worked closely with Rockler throughout the transition to understand USACS performance expectations and communicate them clearly to the Clinicians. USACS also installed a Quality Director for the four EDs to help monitor performance and integrate USACS clinical management tools and other best practices.
The supportive work culture has resulted in outstanding Clinician satisfaction. Twice a year, USACS asks its Physicians and APPs whether they would recommend USACS as an employer. Clinicians rate the practice from 0 to 10 and responses are aggregated into a net promoter score (NPS) that can range from -100 to 100. The June 2025 survey came shortly after USACS had notified several incumbent Clinicians who were not board-certified that in alignment with the health system’s medical staff bylaws, they would soon no longer be eligible to work at these sites. USACS communicated transparently with the Clinicians and offered opportunities at other sites in the region. Even amid this news, every Clinician at the four Arizona EDs who participated in the June NPS survey said they would recommend USACS as an employer, giving the practice the highest possible NPS of 100.
Patients have been more satisfied with their care experience as well. By June, the three hospital EDs had seen an average 33% improvement in patients’ likelihood to recommend the departments, according to Press Ganey survey results. At the freestanding ED, patient NPS scores have exceeded goals since the transition.
“The fact is that the community deserves a safe place to go. My family lives in this city, and I’m proud to now be able to say, ‘Yes, you can go to this hospital—and you can get great care.’” —Senior Clinical Director, Emergency & Trauma Services, USACS Partner Hospital
All of these improvements have helped restore East Valley residents’ confidence in the once struggling EDs. In July, one hospital earned national media attention when the quick actions of the ED team saved the life of a toddler who was bitten twice by a rattlesnake. The hospitals have made strong progress in restoring once-strained relationships with local Emergency Medical Service (EMS) agencies as well. Recent third-party stroke surveys noted local EMS’ confidence in the quality of stroke care at these hospitals. The largest ED is conducting joint trainings and mock drills with EMS and other partners as it pushes to gain Level 1 Trauma certification for the first time in order to elevate the level of care available to the community.
The turn-around of these EDs has also attracted the attention of prospective Clinicians. While several Physicians who cautiously joined USACS part-time during the transition have since expanded to full-time, recruiters have successfully signed many highly qualified local Clinicians who were attracted to USACS’ Physician ownership model. The practice filled remaining vacancies, including those created by the shift to an exclusively board-certified team, by early fall and stood down the STAT Traveling Physicians.
The USACS team and their nursing partners remain focused on achieving length of stay and patient experience goals at all four sites. The key to the successful transition, Rockler says, was collaboration at every level, and clear planning and execution. She describes the nonprofit health system as an ideal partner—organized, agile, and attentive to Clinician needs.
“This hospital system is very dedicated to providing the resources we need to get the job done. They will roll up their sleeves and do their part—and they’ll do it without delay.” —Kendall Rockler, MD, FACEP, Regional Vice President, USACS
The Results
50 % Reduction in Door-to-Clinician Times
ABOUT USACS
ln 2015, the nation’s premier Acute Care Medicine practices formed USACS, a Physician-owned and Physician-led company that set forth a new model for Acute Care Management. Every full-time USACS Physician is offered equity in the company, accounting for 98% of USACS’ ownership and empowering the group to recruit top-quality Clinicians. The remaining 2% is held by health system partners, leaving USACS unencumbered by the volatility of private equity investment. Physician ownership aligns the missions of Clinicians and hospital partners to drive higher standards in quality and value. Today USACS cares for more than 11 million patients annually across more than 400 programs in 27 states.